OVERVIEWAnaesthesia is defined as the temporary loss of any bodily sensation and pain. Anaesthetics are administered by a certified anaesthesiologist, who is responsible for the patient's comfort, safety, and overall condition before, during and after the surgery or any invasive procedure.
Anaesthesia plays a significant role in the perioperative management of cancer patients, which involves the pre-operative care, multidisciplinary cancer care, and post-operative pain management; it also facilitates the patient's early return to the intended oncological therapy (RIOT).
Anaesthetics are either given as an injection, intravenously, inhaled gas, topical spray, patch or even as a liquid.
Types of Anaesthesia
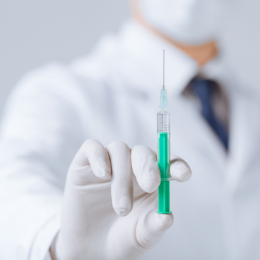
Local anaesthesia is meant for numbing a particular region of the body, like a biopsy. The patient stays awake during the procedure.
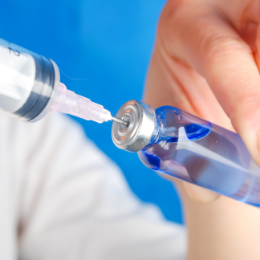
Regional anaesthesia blocks pain in larger parts of the body like arms, legs, or everything below the waist. Despite being conscious, the patient will not be able to move or feel anything in the numbed region, till the effect of anaesthesia wears off.
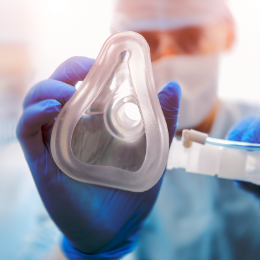
General anaesthesia is recommended during major surgeries. The patient remains unconscious throughout the procedure and gains consciousness as the anaesthesia wears off.
During the procedure, general anaesthesia specialists ensure the comfort and safety of their patients through continuous monitoring.
Anaesthesiology Services at HCG
HCG has a team of expert anaesthesiologists, who are trained exclusively in the field of onco anaesthesia and are skilled at handling cancer patients during high-risk, complex surgeries.
These specialists support cancer patients with preoperative care, intraoperative management, post-operative critical care, and advanced pain management. Our anaesthesia specialists use the evidence-based 'Enhanced Recovery After Surgery (ERAS)' protocols to help patients have shorter hospital stays and return to their routine activities at a faster rate.
With complete pain relief topping their priority, they ensure comfort, faster recovery be it a biopsy or major invasive surgery.

